Shoulder pain can significantly impact daily life, limiting mobility and causing persistent discomfort. For many individuals, when conservative treatments no longer provide relief, shoulder replacement surgery becomes a viable option. In this post, we’ll explore two primary types of shoulder replacement: total shoulder replacement and reverse total shoulder replacement. Understanding the distinctions between these procedures, their indications, and what to expect can empower patients to make informed decisions.
Key Takeaways
- Total shoulder replacement aims to restore the natural anatomy of the shoulder, replacing both the ball (humeral head) and socket (glenoid) components with prosthetic implants.
- Reverse total shoulder replacement reverses the ball-and-socket configuration, placing the ball on the shoulder blade and the socket on the upper arm bone, allowing the deltoid muscle to power arm movement.
- The choice between procedures depends on several factors, including the condition of the rotator cuff, the underlying cause, patient age, activity level, and overall health.
- Both procedures aim to alleviate pain and improve shoulder function, but the recovery process and functional outcomes can differ based on the specific surgery performed.
Understanding Shoulder Anatomy
The shoulder is a complex ball-and-socket joint, one of the most mobile joints in the human body. Three primary bones converge to form the shoulder joint: the humerus (upper arm bone), scapula (shoulder blade), and clavicle (collarbone).
Several soft tissue structures contribute to the shoulder’s stability and function. Articular cartilage is a smooth, slippery tissue that covers the ends of the humeral head and glenoid, allowing them to glide against each other. The rotator cuff is a group of four muscles and their tendons that surround the shoulder joint, important for lifting and rotating the arm, as well as stabilizing the humeral head within the glenoid socket. The large, triangular muscle that covers the shoulder joint, responsible for powerful arm abduction, is called the deltoid.
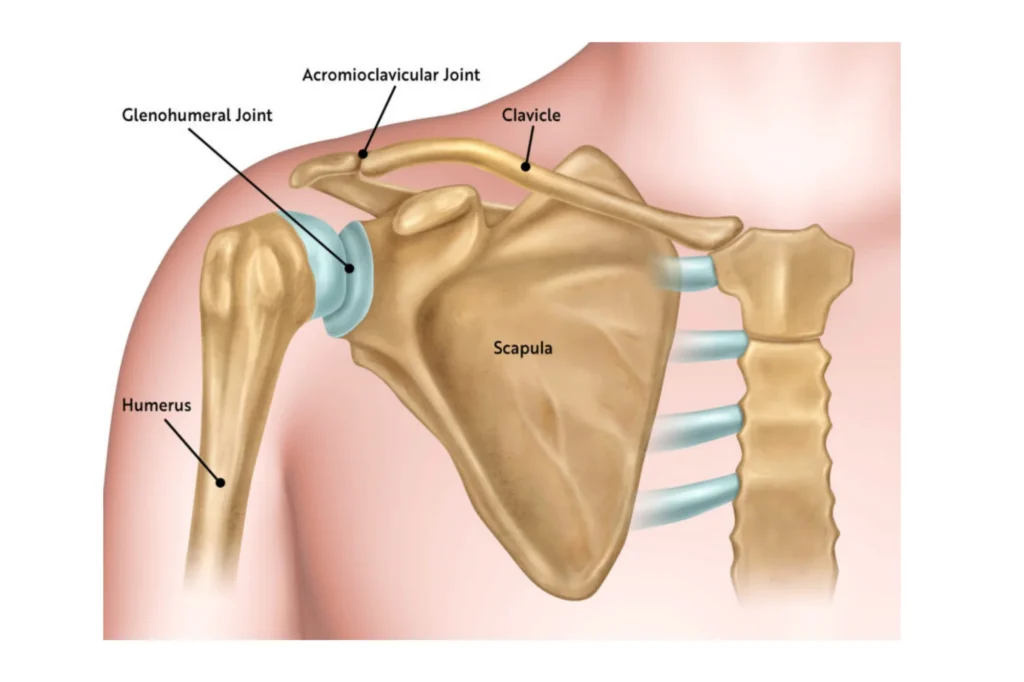
In a healthy shoulder, the intricate interplay of these bones and soft tissues allows for a wide range of pain-free movement. However, when disease or injury compromises these structures, severe pain and functional limitations can arise. An experienced shoulder specialist can evaluate your condition and help recommend if shoulder replacement may be a recommended treatment option for you.
Total Shoulder Replacement: Restoring Natural Anatomy
Total shoulder replacement is a surgical procedure designed to relieve pain and restore function in shoulders severely affected by arthritis or other degenerative conditions, provided the rotator cuff is healthy and intact. In this procedure, the ball and socket are replaced with prosthetic components designed to replicate the natural anatomical structure.

When is Total Shoulder Replacement Recommended?
Total shoulder replacement may be indicated for patients suffering from severe shoulder pain and functional limitations due to:
- Osteoarthritis (Degenerative Joint Disease): This is the most common reason for total shoulder replacement. Over time, the articular cartilage that cushions the ends of the bones may wear away, leading to bone-on-bone friction, pain, stiffness, and loss of motion.
- Rheumatoid Arthritis: An autoimmune disease that causes chronic inflammation of the joints, leading to cartilage destruction and bone erosion.
- Post-traumatic Arthritis: Arthritis that develops after a significant shoulder injury, such as a fracture or dislocation, which damages the joint surfaces and accelerates cartilage degeneration.
- Avascular Necrosis: A condition where the blood supply to the humeral head is disrupted, causing the bone tissue to die and collapse.
- Other Inflammatory Arthropathies: Less common conditions that cause joint inflammation and damage.
Oftentimes, for total shoulder replacement to be successful, the rotator cuff muscles and tendons must be healthy and functional. The rotator cuff plays a key role in stabilizing the shoulder joint and controlling its movement. If the rotator cuff is severely torn or dysfunctional, the procedure may not provide adequate stability or functional improvement, and a reverse total shoulder replacement might be a more appropriate option.
Reverse Total Shoulder Replacement
Reverse shoulder replacement is a specialized procedure that fundamentally alters the biomechanics of the shoulder joint. Unlike total shoulder replacement, which mimics the natural anatomy, reverse total shoulder replacement reverses the ball-and-socket configuration. The design aims to allow patients with severely damaged rotator cuffs to regain significant arm function by relying on the deltoid muscle for movement.

When is Reverse Total Shoulder Replacement Recommended?
Reverse total shoulder replacement is typically reserved for more complex shoulder conditions where a conventional shoulder replacement may not be effective due to a compromised rotator cuff. Primary indications include:
- Cuff Tear Arthropathy: This is the most common indication for reverse total shoulder replacement. The condition can occur when a long-standing, massive, and irreparable rotator cuff tear leads to severe arthritis and superior migration of the humeral head.
- Massive, Irreparable Rotator Cuff Tears: Even without advanced arthritis, patients with large, chronic rotator cuff tears that cannot be surgically repaired may benefit from reverse shoulder replacement.
- Complex Shoulder Fractures: Severe fractures of the humeral head that are not amenable to repair, especially in older patients with poor bone quality or compromised rotator cuffs, may be treated with reverse total shoulder replacement.
By reversing the ball and socket, the reverse total shoulder replacement shifts the center of rotation of the shoulder, placing the deltoid muscle in a more advantageous position to lift and move the arm, even in the absence of a functional rotator cuff.
The Replacement Procedures: What to Expect
The procedures typically involve the following steps:
- Anesthesia: The patient receives general anesthesia, often combined with a regional nerve block, to ensure comfort during and after surgery.
- Incision: An incision is made to access the joint.
- Site Preparation: The damaged components are removed, and the sites are prepared to receive the prosthetic components.
- Implant Placement: The new ball and socket components are carefully positioned. In total shoulder replacement, they restore the natural anatomy of the shoulder joint. In reverse replacement, the positioning of the ball and socket is reversed.
- Closure: The incision is closed, and a sterile dressing is applied.
Recovery and Rehabilitation
Recovery after both procedures typically follows a structured rehabilitation program, though the focus of the program may differ.
Key aspects of recovery may include:
- Immobilization: The arm is usually placed in a sling for several weeks to protect the healing tissues and allow the shoulder to rest.
- Physical Therapy: Rehabilitation focuses on regaining motion and strength. For patients who received a reverse shoulder replacement, added focus is placed on strengthening the deltoid muscle. Initially, passive and active-assisted range of motion exercises are performed, with a gradual progression to strengthening exercises.
- Activity Restrictions: Patients may have specific restrictions to protect the implant and prevent dislocation. Heavy lifting and certain overhead activities may be restricted or modified. Your surgeon and physical therapist will provide detailed guidance on safe activities.
Summary
Total shoulder replacement and reverse total shoulder replacement are both surgical interventions designed for alleviating shoulder pain and improving function, but they may be recommended for distinct patient populations and conditions. Total shoulder replacement may be the preferred option for individuals with severe shoulder arthritis and an intact rotator cuff, aiming to restore the shoulder’s natural anatomy and mechanics. In contrast, reverse total shoulder replacement offers a solution for patients with compromised rotator cuffs, cuff tear arthropathy, or complex fractures, by reversing the joint’s ball-and-socket configuration to leverage the deltoid muscle for movement.
Choosing the right procedure requires a thorough evaluation by an experienced orthopedic surgeon. While both surgeries involve a dedicated recovery and rehabilitation process, the long-term benefits of pain relief and improved quality of life can be profound for many patients. If you are experiencing persistent shoulder pain and functional limitations, consulting with a shoulder specialist is the first step towards understanding your options and embarking on the path to recovery.
Frequently Asked Questions
How long does shoulder replacement surgery take?
The surgical procedure itself typically takes between 1 to 3 hours, depending on the complexity of the case and the type of replacement. This does not include preparation and recovery time in the operating room suite.
How painful is shoulder replacement surgery?
While shoulder replacement is a major surgery, significant advancements in pain management techniques, including regional nerve blocks, have made the post-operative period more manageable. Patients will experience discomfort, but it can typically be well-controlled.
When can I return to normal activities after shoulder replacement?
The timeline for returning to normal activities can vary significantly between individuals and depends on the type of surgery and adherence to rehabilitation. Light daily activities can often resume within a few weeks, but returning to more strenuous activities, sports, or heavy lifting can take 6 months to a year or even longer. Your surgeon and physical therapist can provide a personalized timeline.
Can I play sports after shoulder replacement?
Many patients can return to low-impact sports and activities like golf, swimming, and cycling after shoulder replacement. High-impact sports, contact sports, and activities involving heavy lifting or repetitive overhead movements may need to be avoided or modified to protect the implant. Your surgeon will provide specific recommendations based on your individual case and the type of replacement.





